What is the normal range for DLCO VA

Zoe Patterson
Published Apr 23, 2026
Normal DLCO: >75% of predicted, up to 140% Mild: 60% to LLN (lower limit of normal) Moderate: 40% to 60% Severe: <40%
What is a normal DLCO VA?
The corrected value is referred to as the DLCO/VA and a normal value is considered to be 80% or more of the predicted value.
What is abnormal DLCO?
Dlco is a specific but insensitive predictor of abnormal gas exchange during exercise. Low Dlco less than or equal to 50% predicted can predict hypoxemia with exercise. A normal Dlco does not rule out oxygen desaturation with exercise.
What is DLCO VA in a PFT?
The diffusing capacity of the lung is usually reported as both the diffusing capacity (DLCO) and the diffusing capacity divided by the alveolar volume (DLCO/VA).What does low DLCO indicate?
A reduced DLCO and a reduced KCO suggest a true interstitial disease such as pulmonary fibrosis or pulmonary vascular disease. It has demonstrated that in healthy patients, the KCO is increased to above normal levels when the DLCO test is performed at volumes less than the TLC.
Does DLCO decrease with age?
DLCO decreases with age, as does resting arterial oxygen tension (PaO2). Reference equations specific for age have been established, but in general, PaO2 <70 mmHg is abnormal.
Can you improve DLCO?
Conclusion: Pulmonary rehabilitation improves oxygenation, severity of dyspnea, exercise capasity and quality of life independent of carbon monoxide diffusion capacity in patents with COPD. Improvement in DLCO in patients with severe diffusion defect suggests that pulmonary rehabilitation reduced mortality.
What is normal RV TLC ratio?
VariableMeanStandard DeviationRV Actual2.31 (119%)0.68TLC Actual5.43 (98%)1.28RV/TLC Ratio42.708.47Diffusion Capacity % Predicted85%12.1Is DLCO normal in asthma?
Average DLCO values were normal in the asthma group (103%P) and lower in the COPD (69%).
How is low lung volume treated?- Inhalers.
- Immunosuppressants.
- Expectorants.
- Oxygen therapy.
- Pulmonary rehabilitation.
- Lung transplant.
- Other treatments.
- Restrictive vs. obstructive lung diseases.
What is decreased diffusing capacity in a lung?
In practice, the diffusing capacity is commonly decreased in three categories of disease in which surface area for gas exchange is lost, pulmonary capillary blood volume is decreased, or both: (1) emphysema, (2) diffuse parenchymal lung disease, and (3) pulmonary vascular disease.
Why is DLCO low in pulmonary fibrosis?
DLCO values represent the ability of the lung to transfer gas from the inhaled air into the blood stream and acts as a surrogate marker of the extent of lung damage (1). DLCO values may decrease because of several clinical conditions including emphysema, interstitial lung diseases, or pulmonary fibrosis (2).
Why is DLCO low in pulmonary hypertension?
In patients with PAH, the primary cause of a low DLCO is a reduction in the pulmonary capillary blood volume, whereas in patients with IPF- PH, disorder/thickening of the alveolar to capillary membrane reduces the DLCO.
Why DLCO is increased in asthma?
Asthma & DLco The high DLCO values [123, 124] have been explained by hyperinflation, increased intrathoracic pressure, and a more likely cause, increases in pulmonary capillary blood volume or extravasation of red blood cells into the alveolus.
Why is DLCO low in COPD?
In COPD, the DLCO decreases with increasing severity of disease. This is because in emphysema, the lung has lost alveoli, resulting in a lower surface area available for diffusion. In addition, there is also a loss of capillary bed, which can also decrease DLCO.
Is DLCO normal in pulmonary fibrosis?
Conclusions: One in four patients with IPF had normal TLC and more than one-half had a normal FVC during initial evaluation. As the severity of the restriction increased, FEV1⁄FVC increased, DLCO decreased but DLCO⁄VA remained normal.
How is DLCO performed?
Diffusing capacity (DLCO) is most commonly measured using the single-breath technique. The patient takes a full inspiration of a gas mixture containing 0.3 percent carbon monoxide and 10 percent helium (the dilution of which provides an index of lung or “alveolar” volume).
What triggers dyspnea?
According to Dr. Steven Wahls, the most common causes of dyspnea are asthma, heart failure, chronic obstructive pulmonary disease (COPD), interstitial lung disease, pneumonia, and psychogenic problems that are usually linked to anxiety.
What should my lung capacity be?
Lung capacity or total lung capacity (TLC) is the volume of air in the lungs upon the maximum effort of inspiration. Among healthy adults, the average lung capacity is about 6 liters.
How can I test my lung capacity at home?
- Set the pointer. …
- Attach the mouthpiece to the meter. …
- Sit up or stand up as straight as you can, and take a deep breath.
- Close your lips tightly around the mouthpiece. …
- Breathe out as hard and as fast as you can for 1 or 2 seconds. …
- Write down the number on the gauge. …
- Repeat these steps 2 more times.
What vitamins are good for your lungs?
Taking certain dietary supplements, including, vitamin C, vitamin D, magnesium, omega-3s, zinc, and selenium may also help promote lung health, especially among those with conditions that affect the lungs, such as COPD, asthma, and certain forms of cancer.
What are low lung volumes?
Low lung volume If your lung volume is lower than normal, this may be a sign of a restrictive lung condition such as pulmonary fibrosis or sarcoidosis.
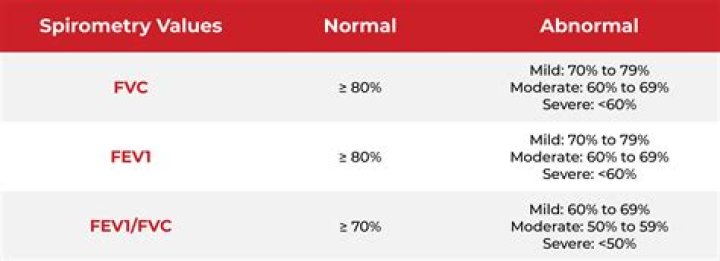
What are normal values for spirometry test results?
Percentage of predicted FEV1 valueResult80% or greaternormal70%–79%mildly abnormal60%–69%moderately abnormal50%–59%moderate to severely abnormal
What does 60 percent lung capacity mean?
60-69% 50-59% less than 50% Restrictive lung diseases can cause the FVC to be abnormal. This means that the lung is restricted from filling to its normal capacity of air.
What is the life expectancy of a person with interstitial lung disease?
The average survival for people with this type is currently 3 to 5 years . It can be longer with certain medications and depending on its course. People with other types of interstitial lung disease, like sarcoidosis, can live much longer.
What are signs of lung failure?
- difficulty breathing or shortness of breath, especially when active.
- coughing up mucous.
- wheezing.
- bluish tint to the skin, lips, or fingernails.
- rapid breathing.
- fatigue.
- anxiety.
- confusion.
What is high DLCO?
Conclusion: A high DLCO on a PFT is most frequently associated with large lung volumes, obesity, and asthma. Other conditions are much less common. A clinical condition, which typically reduces DLCO, may deceptively normalize DLCO in such patients.
How do you increase diffusion capacity in lungs?
Deep breathing exercises may help increase lung capacity. For instance, the British Lung Foundation say that deep breathing can help clear mucus from the lungs after pneumonia, allowing more air to circulate. To perform this exercise: Breathe deeply 5–10 times, then cough strongly a couple of times, and repeat.
Can PFT detect pulmonary hypertension?
PFT results suggestive of pulmonary hypertension Along with identifying other lung diseases, there are specific findings that are consistent with a diagnosis of pulmonary hypertension such as a low diffusing capacity without other abnormalities.
Does pulmonary hypertension affect lung capacity?
Spirometry and expiratory flow. 20-40% of patients with IPAH have airway obstruction based on a forced expiratory volume in 1 second to forced vital capacity (FEV1/FVC) ratio of less than 70% [19], [27]. The overall mean FEV1/FVC ratio is significantly reduced at 76% compared to 84% in controls (p < 0.001) [22].
How does pulmonary hypertension affect lung function?
In one form of pulmonary hypertension, called pulmonary arterial hypertension (PAH), blood vessels in the lungs are narrowed, blocked or destroyed. The damage slows blood flow through the lungs, and blood pressure in the lung arteries rises. The heart must work harder to pump blood through the lungs.



