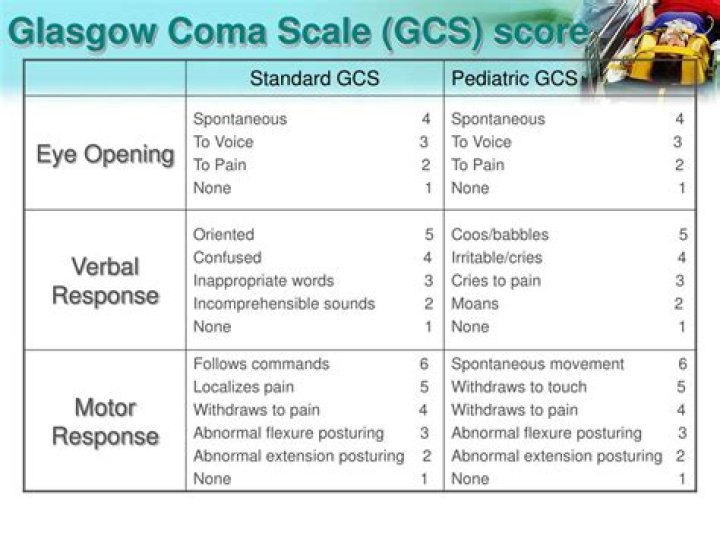
What is a normal GCS score

Zoe Patterson
Published Apr 22, 2026
A normal GCS score is equal to 15, which indicates a person is fully conscious.
What does a GCS score of 15 mean?
The GCS is often used to help define the severity of TBI. Mild head injuries are generally defined as those associated with a GCS score of 13-15, and moderate head injuries are those associated with a GCS score of 9-12. A GCS score of 8 or less defines a severe head injury.
Is a GCS of 15 good?
Head Injury Classification: Severe Head Injury—-GCS score of 8 or less Moderate Head Injury—-GCS score of 9 to 12 Mild Head Injury—-GCS score of 13 to 15 (Adapted from: Advanced Trauma Life Support: Course for Physicians, American College of Surgeons, 1993).
What does a GCS of 7 mean?
Certain scores on the Glasgow Coma Scale have significance. Patients with a Glasgow Coma Scale score of 7 or less are considered comatose. Patients with a Glasgow Coma Scale score of 8 or less are considered to have suffered a severe head injury.What does a GCS of 11 mean?
Every brain injury is different, but generally, brain injury is classified as: Severe: GCS 8 or less. Moderate: GCS 9-12. Mild: GCS 13-15.
What does GCS 14 mean?
The GCS is the summation of scores for eye, verbal, and motor responses. The minimum score is a 3 which indicates deep coma or a brain-dead state. The maximum is 15 which indicates a fully awake patient (the original maximum was 14, but the score has since been modified).
What does a GCS of 10 mean?
For example, a score of 10 might be expressed as GCS10 = E3V4M3. Best eye response (4) No eye opening. Eye opening to pain. Eye opening to sound.
Can you recover from a GCS of 7?
4 The survival rate after a TBI, severe enough to cause deep coma and low Glasgow Coma Scale (GCS) scores, is generally poor, even in young adults. Studies show a very high overall mortality, ranging between 76% and 89%. 5, 6, 7 Of the surviving patients, only very few recover to a good outcome.What does a GCS of 3 mean?
Patients with head injury with low Glasgow Coma Scale (GCS) scores on hospital admission have a poor prognosis. A GCS score of 3 is the lowest possible score and is associated with an extremely high mortality rate, with some researchers suggesting that there is no chance of survival.
How do you calculate GCS?To calculate the patient’s GCS , you need to add together the scores from eye opening, verbal response and motor response. Added together, these give you an overall score out of the maximum of 15.
Article first time published onAt what GCS do you intubate?
In trauma, a Glasgow Coma Scale score (GCS) of 8 or less indicates a need for endotracheal intubation. Some advocate a similar approach for other causes of decreased consciousness, however, the loss of airway reflexes and risk of aspiration cannot be reliably predicted using the GCS alone.
What GCS is unconscious?
A score of 3 is indicative of a deep level of unconsciousness and 15 means that the person is fully alert. These scores are used to predict early mortality and longer term outcome in patients following Acquired Brain Injury. The GCS is one of the measures used to assess severity of injury.
What are the stages of a coma?
Three stages of coma DOC includes coma, the vegetative state (VS) and the minimally conscious state (MCS).
What does a GCS of 13 indicate?
A GCS of 8 or less indicates severe injury, one of 9-12 moderate injury, and a GCS score of 13-15 is obtained when the injury is minor.
When do you use the Glasgow Coma Scale?
The GCS was initially used to assess level of consciousness in patients after head injury, but the scale is now used in many acutely unwell patients. In hospitals it is also used to monitor patients in intensive care units.
What is GCS nursing?
Glasgow Coma Scale (GCS) is a reproducible tool used by nurses in almost every healthcare facility to assess level of consciousness in a patient with a neurological problem. It is important to have the skill and knowledge when assessing and applying critical thinking to interpret the findings.
What does a Glasgow Coma Scale score of 5 indicate?
In the case of GCS scores of 3 to 5, mortality is high and success has generally been low, whereas for GCS scores of 6 to 8, aggressive triage and neurosurgical management may be the most important determinant of outcome.
What is the range of a normal total score on the Glasgow Coma Scale quizlet?
The range of scores for the Glasgow Coma Scale is 3 to 15.
Can a person recover from GCS 3?
However, even after severe brain injuries, recovery is possible. According to one comprehensive study of 189 patients with a GCS score of 3, 13% achieved a good functional outcome after six months.
What is a GCS of 3t?
Threshold to consider intubation for airway protection (ATLS) = 8. Intubated patients are given a “t” for verbal, denoted as “GCS 3t”
What is the longest time someone was in a coma and woke up?
Terry Wallis (born 1964). This American man was in a coma for nearly a year after a truck accident, then a minimally conscious state for 19 years.
How do you tell if someone is coming out of a coma?
Signs of coming out of a coma include being able to keep their eyes open for longer and longer periods of time and being awakened from “sleep” easier—at first by pain (pinch), then by touch (like gently shaking of their shoulder), and finally by sound (calling their name).
What percent of coma patients wake up?
They found that those who showed less than 42 percent of normal brain activity didn’t regain consciousness after a year, while those who had activity above that woke up within a year. Overall, the test was able to accurately predict 94 percent of patients who would wake up from a vegetative state.
What is normal flexion in GCS?
Withdraws to pain (4 points) This response is also referred to as a “normal flexion response” as the patient typically flexes their arm rapidly at their elbow to move away from the painful stimulus.
Is intubated and ventilated the same thing?
Intubation is placing a tube in your throat to help move air in and out of your lungs. Mechanical ventilation is the use of a machine to move air in and out of your lungs.
What meds are used for intubation?
[4] Common sedative agents used during rapid sequence intubation include etomidate, ketamine, and propofol. Commonly used neuromuscular blocking agents are succinylcholine and rocuronium. Certain induction agents and paralytic drugs may be more beneficial than others in certain clinical situations.
How do you perform RSI?
- Plan.
- Preparation (drugs, equipment, people, place)
- Protect the cervical spine.
- Positioning (some do this after paralysis and induction)
- Preoxygenation.
- Pretreatment (optional; e.g. atropine, fentanyl and lignocaine)
- Paralysis and Induction.
- Placement with proof.
Do you have a pulse when you're unconscious?
They may be unconscious for a few seconds — as in fainting — or for longer periods of time. People who become unconscious don’t respond to loud sounds or shaking. They may even stop breathing or their pulse may become faint. This calls for immediate emergency attention.
What motor response means?
Motor Response – Obeys commands You must get the patient to follow a simple command such as stick your tongue out or lift up your right arm. This would score 6. Asking the patient to squeeze your hands should be avoided as this might elicit a reflex squeezing rather than the obeying of a command.
How long can you be in a coma before brain damage?
If this condition persists for more than four weeks they can be classified as being in a continuing vegetative state. If it continues for 12 months after traumatic brain injury or 6 months after non-traumatic brain injury, the person can be classed as being in a permanent vegetative state.
How long can someone be in a coma and still wake up?
Over time, the person may start to gradually regain consciousness and become more aware. Some people will wake up after a few weeks, while others may go into a vegetative or minimally conscious state.



